Many cardiovascular issues including dysautonomia can be corrected, or partially so, by appropriate nutrition or the clever use of nutrients as well as exercise i.e. relatively simple lifestyle and habit modifications.
LEARN ABOUT OUR KIDS IN ACTION AND ATHLETES IN ACTION NUTRITION AND FITNESS PROGRAM
Eat a healthy diet with frequent meals of a low-glycemic-index diet
 Eat 5 meals a day; breakfast, lunch and dinner and two snacks in between. Make sure there is protein and fat in every meal. Make sure the carbohydrate chosen is complex and slowly digestible. The idea is to eat in such a way that blood glucose is maintained evenly throughout the day and minimal insulin is released from the pancreas. Swings in blood glucose increase vasovagal symptoms. For those that do not have many GI symptoms, a very good example of a diet that helps manage vasovagal syncope well is The South Beach Diet.
Eat 5 meals a day; breakfast, lunch and dinner and two snacks in between. Make sure there is protein and fat in every meal. Make sure the carbohydrate chosen is complex and slowly digestible. The idea is to eat in such a way that blood glucose is maintained evenly throughout the day and minimal insulin is released from the pancreas. Swings in blood glucose increase vasovagal symptoms. For those that do not have many GI symptoms, a very good example of a diet that helps manage vasovagal syncope well is The South Beach Diet.
For those with evidence of GI dysmotility, I recommend a modification of the South Beach Diet to include the rules of the low-FODMOP diet. See the addendum at the back of this piece. Our ‘Kids in Action/Athletes in Action‘ Program nutritionists can guide patients with their diet and activity. See details of this program
Please see these documents in the addendum for more information on Diet and Supplements:
Supplements
In addition to diet there are many supplements that can bring additional benefits.
For more information please refer to the Nutritional Supplement section
Hydrate Well
This is with water or flavored waters that have no sugars added. The amount required to hydrate varies with metabolism, activity level and environment.
A typical adolescent would be required to drink three 750 ml bottles of water each day in addition to what they normally drink at meal times. If they work-out, they need to drink more.
One can judge if they are well hydrated if they need to go to the bathroom several times a day and their urine is diluted (clear, not concentrated).

3 bottles on an inactive day, more if working out or sweating a lot
Salt Addition
 If one is eating a typical Western Diet which includes frequent fast foods and processed food, one is not eating the type of diet described above and is already taking in excessive amounts of salt. However, when one eats consistently healthily with fresh fruits, vegetables, meats, fish, and dairy, and whole grains, salt in the diet is much less and addition of salt may improve symptoms. This is a recommendation for young, healthy people with normal blood pressure and its because they have such pliable blood vessels that they are able to tolerate salt well and indeed need it added to their diet.
If one is eating a typical Western Diet which includes frequent fast foods and processed food, one is not eating the type of diet described above and is already taking in excessive amounts of salt. However, when one eats consistently healthily with fresh fruits, vegetables, meats, fish, and dairy, and whole grains, salt in the diet is much less and addition of salt may improve symptoms. This is a recommendation for young, healthy people with normal blood pressure and its because they have such pliable blood vessels that they are able to tolerate salt well and indeed need it added to their diet.
 When a person becomes older, and their blood vessels become stiff, they need to avoid salt as it causes hyperten- sion. The sources of salt in the diet should be carefully chosen. It should not come from unhealthy snack foods like French fries or potato chips but rather from nuts and sunflower seeds.
When a person becomes older, and their blood vessels become stiff, they need to avoid salt as it causes hyperten- sion. The sources of salt in the diet should be carefully chosen. It should not come from unhealthy snack foods like French fries or potato chips but rather from nuts and sunflower seeds.
The exact amount of salt to add and its affect at relieving symptoms is different for each person. Experts in autonomic dysfunction believe that 4 to 7 grams of salt per day is needed to manage this issue but varies with salt metabolism, activity level and environment – basically, how quickly one loses salt through sweat. One should aim closer to 7 grams per day if one sweats a lot with activities and work-out often.
Often times, this amount of salt cannot be obtained from snacks and by salting one’s food and that is when salt tablets become handy.
Thermatabs are a recommended buffered salt tablet.

For more information on Salt Suppleements please refer to outr list of Supplemental Salt & Electrolyte Water section
Good Sleep Habits
 A full night’s restful sleep helps reduce symptoms of vasovagal hyper-reactivity. For adolescents, this means 8 to 10 hours of sleep each night. In my experience, restful sleep is often disrupted in patients with autonomic dysfunction and all efforts need to be made to restore this.
A full night’s restful sleep helps reduce symptoms of vasovagal hyper-reactivity. For adolescents, this means 8 to 10 hours of sleep each night. In my experience, restful sleep is often disrupted in patients with autonomic dysfunction and all efforts need to be made to restore this.
Helpful techniques include implementing a consistent nighttime routine that includes a consistent bedtime, starting one hour before bedtime, begin strict avoidance of all electronic screens (computers, tv, cellphones), drinking herbal tea, and taking melatonin 1 to 10mg each night.
Consistent Aerobic and Strength Training Exercise
Exercise such as running, biking, swimming, or even brisk walking, if its done a regular basis, likely tones the blood vessels and makes them less likely to dilate inappropriately. Strength training exercises designed to strengthens the ‘muscle pumps’ in the lower half of the body helps maintain blood volume in the upper half of the body when standing.

I strongly recommend at least 30 minutes of aerobic activity where the heart rate is maintained at 150 beats per minute for the duration of exercise. That means that if you were to take your pulse during exercise for a 6 second count, your pulse should be 15 beats during the 6 seconds.

For those with Grade III dysautonomia, a regimented exercise program beginning with recumbent exercises including recumbent bike, rowing and swimming with the aid of a physical therapist are strongly recommended. A 6-month advancing training schedule is given in as an addendum.
Typical Excercise Information
To view a typical recommended exercise routine checkout the Levine Protocol Example in the addendum.
Physical Thereapy
Below is a a sample physical therapy prescription.
You can view a map of physical therapists, along with contact information, on our site by visiting here: Specialty Physical Theraptists in the Bay Area
Use of Compression Garments
Calf stockings and thigh-high tights. Arm sleeves may be added for additional effect. These should be fitted to produced 20 to 40 mmHg of compression as measured by pedal Doppler with lower calf manual BP cuff with and without garments.



Ideally, these should be fitted for pressure-effect prior to purchase so our Compression Garments document in the addendum for types, brands and physical and web addresses to purchase.
Recognition of Early Symptoms
 Progression of vasovagal symptoms to syncope can be aborted if the early symptoms are recognized and acted on. Whenever lightheadedness advances to a change in vision or hearing, lie down flat immediately to get the head and heart at the same level. Gravity is then out of the equation and blood flow to the brain is restored. It’s even better to raise the legs against a wall or placed on a chair to help further drain blood toward the head. While this might seem embarrassing to suddenly lie down in front of friends and school mates, it is much safer and less embarrassing than fainting. Also, it saves calls to 911 and trips by ambulance to the emergency room as well as costly head MRIs.
Progression of vasovagal symptoms to syncope can be aborted if the early symptoms are recognized and acted on. Whenever lightheadedness advances to a change in vision or hearing, lie down flat immediately to get the head and heart at the same level. Gravity is then out of the equation and blood flow to the brain is restored. It’s even better to raise the legs against a wall or placed on a chair to help further drain blood toward the head. While this might seem embarrassing to suddenly lie down in front of friends and school mates, it is much safer and less embarrassing than fainting. Also, it saves calls to 911 and trips by ambulance to the emergency room as well as costly head MRIs.
Avoidance of Activities that Worsen Symptoms
Avoid exposure or at least vigorous activities in hot weather. Avoid hot showers. Avoid sudden head-up postural changes, Avoid prolonged recumbency, Avoid large heavy meals, Avoid alcohol. Avoid caffeine. Avoid over-doing activities such as late night partying with friends and pushing oneself on weekends to keep up with friends. These usually lead to set-backs that can have repercussions the rest of the week.
Use of Physical Counter-maneuvers
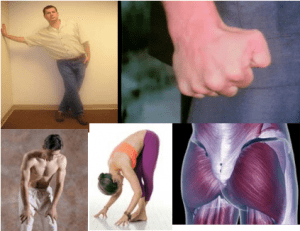
When vasovagal symptoms strike and lying down is not possible, then move around to use leg muscles. Do activities as such as:
- leg crossing
- bending forward
- placing a foot on a chair
- making fists
- active contraction of abdominal and buttock muscles
Avoidance of Medications that Worsen Symptoms
Many drug classes can unmask or worsen the symptoms of autonomic dysfunction and should be withdrawn if possible or avoided if considered for other reasons. A list of these classes is given in the table.